This is one of the many true stories of genetic counseling. I saw this couple early last year and they are on my mind today because they called me last night. I am changing their names because, like all good genetic counselors, I respect confidentiality and privacy. I am sharing their story because every newlywed can learn from their story.
Samir and Anne had fought against all kinds of odds as a couple- religious differences, financial difficulties, career crises, and everything else in between. Nevertheless, when I saw them at their appointment, none of those struggles mattered to either one of them. They were happily married for a year, their respective families had finally come around to seeing in them what they saw in each other, proud owners of an extremely successful startup in the food industry, and knew they were already in love with their baby growing in Anne’s belly. They would do “anything”, they said, to ensure the baby was fine and, would love the baby no matter what. So what brought them to genetic counseling? Both, turns out, had blood reports that indicated they might be a carrier of beta thalassemia.
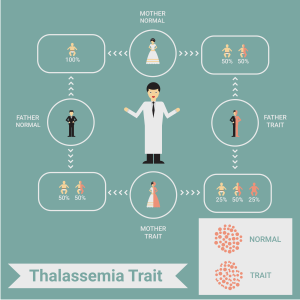
What is beta thalassemia?
It is a common (especially in India) genetic and inherited disorder of the blood in which the body has trouble producing regular hemoglobin. Hemoglobin is the part of red blood cells that carries oxygen throughout the body. The abnormal hemoglobin results in red blood cells getting destroyed at a very fast rate, and this leads to anemia. Anemia is a condition in which the body doesn’t have enough normal, healthy red blood cells and can result in:
- Chronic fatigue. Severe anemia can cause a heightened level of tiredness that can come in the way of even simple tasks of everyday living.
- Heart problems. Anemia can lead to irregular or rapid heartbeat. Having anemia forces the heart to pump harder and faster in order to make up for oxygen deficits. This elevated heart rate is burdensome to the heart and can, in turn, lead to an enlarged heart or even heart failure.
- Pregnancy complications. Pregnant women with anemia are more likely than those without anemia to experience complications including premature delivery
- Death. Some types of genetic anemias can be serious and life-threatening. Extreme and rapid blood loss results in acute, severe anemia which can be fatal.
Back to Samir and Anne. Neither of them had thalassemia but were at high risk for being carriers. The possibility never even crossed their mind, as they had always enjoyed good health and were certain they weren’t related to each other in any way. Here is where we had to work together very quickly because they were over 3 months pregnant, their risk for being a carrier of beta thalassemia was high, their actual genetic carrier status was not known, and time was ticking. These are learnings from their genetic counseling appointment:
- From family history assessment, it was uncovered that Samir belongs to a specific community in Gujarat which is known to have an increased frequency of carriers of thalassemia. In India, about 4 crore people are silent carriers of thalassemia and about 10,000 babies are born with beta thalassemia each year. Rajkot, Jamnagar and Surat have the highest incidence of thalassemia in India, followed by the states of Haryana, Bengal and Orissa.
Public awareness, carrier screening, and genetic counseling are key- during pregnancy and especially before conception.
- Since their risks for being a carrier was brought to light from a regular Complete Blood Test (CBC) showing Mean Corpuscular Volume (MCV) less than 90, hemoglobin electrophoresis was immediately ordered, we had the results in a week that confirmed both Samir and Anne were carriers of beta thalassemia.
Routine CBC with a focus on MCV can be an invaluable carrier screen for thalassemia and any couple that has low MCVs, must proceed to get hemoglobin electrophoresis
- During their personal and emotional genetic counseling appointment, 3 available options were discussed here:
- Option 1: Samir and Anne could get a genetic test to determine the exact change in their genes that we would, later, look for in the developing baby with an amniocentesis – a procedure that allows for the collection of cells that represent the developing baby. If the baby had the gene change from Samir as well as the gene change from Anne, it would have thalassemia. If the baby had only either one of the gene changes (either from Samir or from Anne), it would be a healthy carrier exactly like its parents. Samir and Anne shared that they would continue the pregnancy even if the developing baby was going to have thalassemia. They were clear that they would be able to handle regular transfusions every 2 weeks for their child, and a cost of Rs.5000 (approx.) per transfusion. They were not going to change their mind about bringing this baby into the world.
- Option 2: Get an amniocentesis immediately and send the sample, along with their blood samples, for genetic testing all at the same time. This way we would know the gene change that Anne and Samir had, and would be able to look for them concurrently in the developing baby.
- Option 3: Because they would not change the course of pregnancy as termination was never going to be an option for them, they could also choose to not have genetic testing for thalassemia at all. (For those of you reading this who cannot imagine why someone wouldn’t want to know genetic status of their baby, here are some reasons from parents who decided to not have genetic testing for inherited blood disorders.
Prenatal (and preconception) genetic counseling is an extremely personalized healthcare specialty that focuses on the individual, their values, their beliefs and helps couples understand complex genetics concepts and make important medical decisions that’s good for them.
So what did they choose? Samir and Anne decided that although they would not change the course of the pregnancy, they wanted to know as much as they could about the developing baby and themselves so that they may best take care of their new family. They chose to:
- Get genetic carrier testing for thalassemia for themselves in order to share this information with their families. They had siblings and cousins who were planning on having babies and wanted to do the right thing for their families. They chose to not get an amniocentesis because they would not terminate the pregnancy.
- Schedule a genetic newborn screening (NBS) test for their child at birth to test for not just thalassemia, but several other conditions that can be easily managed with early diagnosis and intervention
It’s always important to understand that different people make different choices in similar situations because each one has different beliefs, values, experiences, support systems, coping strategies, influences in life. There is no “one right answer” to some of life’s bigger questions about who “deserves” the right to live, and what really is “normal”. I made sure they fully understood the implications of their decision, and told them to stay in touch if anything changes for them, or even if they just wanted to stay in touch.
Which brings me back to why Samir and Anne are on my mind today.
Last year, they had an emotionally rough pregnancy, chose to continue with it, had a baby whose genetic newborn screening test came back positive for thalassemia, started their baby on transfusions and chelation therapy, went global with their start up, and sent me many pictures. Last night, they called to invite me for a party – they were celebrating Sanaya’s 1st birthday and wanted me to be a part of it. I couldn’t have asked for a greater honor. Or a better job.